Hantavirus: What It Is, How It Spreads, and Why It's So Deadly
It spreads through rodent droppings, has no vaccine or antiviral, and depends on an ICU response that rural communities may never reach in time.
From the Korean War to the Four Corners: how hantavirus was discovered.
The virus makes blood vessels leak, and the immune system makes it worse.
The most important diagnostic question: have you been around mice or rats?
There is no cure. Survival depends on ICU support and timing.
Rodent-proofing is cheap, proven, and more reliable than protective gear.
Each outbreak revealed something new about how the virus spreads.
Animal-waste diseases cause 450,000 infections in the U.S. each year.
The agency responsible for tracking these diseases lost a third of its staff.
From the Korean War to the Four Corners: how hantavirus was discovered.
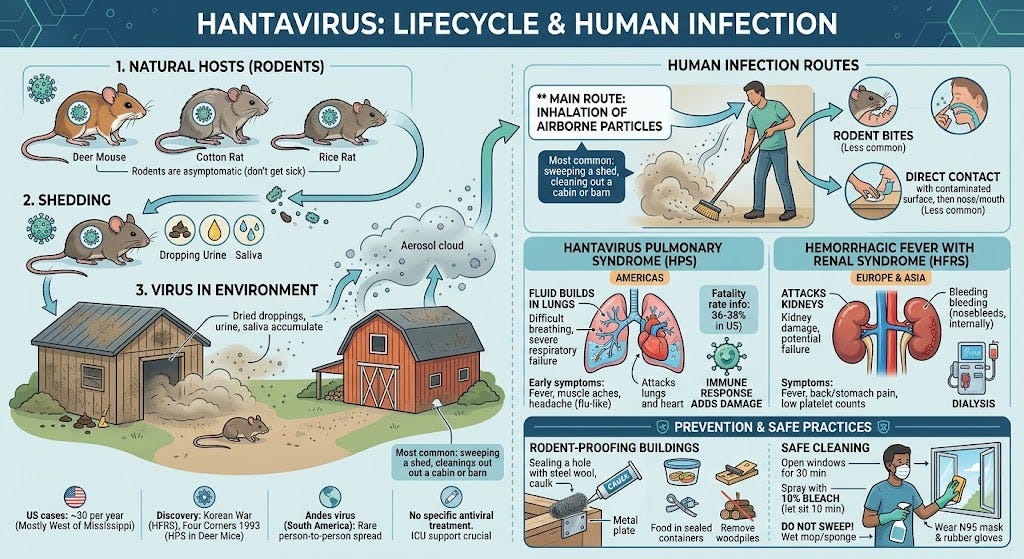
Hantavirus is a family of viruses carried by rodents like mice and rats. The animals don’t get sick from it. They shed the virus in their urine, droppings, and saliva.
The virus was first recognized during the Korean War, when over 3,000 United Nations troops fell ill with a mysterious kidney disease. Scientists didn’t isolate the virus until 1978. They named it after the Hantan River in South Korea, near the demilitarized zone where the soldiers were stationed.
The American form of the disease — hantavirus pulmonary syndrome, or HPS — was discovered in 1993 after a cluster of young, healthy people in the Four Corners region of the Southwest died of sudden lung failure. Investigators traced the cause to a previously unknown virus carried by deer mice.
There are two main diseases hantavirus causes, depending on the strain:
Hantavirus pulmonary syndrome (HPS) is found in the Americas. It attacks the lungs and heart. The case fatality rate ranges from 12% to 45%, depending on the strain. In the United States, it has averaged around 36% to 38%.
Hemorrhagic fever with renal syndrome (HFRS) is found in Europe and Asia. It attacks the kidneys. The fatality rate ranges from less than 1% to about 15%, depending on the strain.
Worldwide, an estimated 200,000 to 300,000 people are infected each year. More than half of the kidney form are in China. In the Americas, about 300 cases of the lung form are diagnosed annually, mostly in Argentina, Brazil, and Chile.
There is no approved vaccine in the Americas or Europe. There is no antiviral drug that works for the lung form.
Sweeping a shed is the most common way people catch it.
People catch hantavirus by breathing in tiny particles from dried rodent urine, droppings, or saliva. This usually happens when someone disturbs an area where mice or rats have been living: sweeping a shed, cleaning out a cabin, opening a barn that’s been closed up, or moving stored boxes or firewood.
The virus can also spread through a rodent bite or by touching a contaminated surface and then touching your nose or mouth. These routes are less common.
The incubation period — the time between exposure and getting sick — is 9 to 33 days, with a median of about two weeks.
Almost all hantaviruses spread only from rodents to people. The one exception is the Andes virus in South America, and a person can be contagious before symptoms begin. The virus has been detected in blood up to two weeks before symptom onset, and in saliva and nasopharyngeal secretions during the early stages of infection. The risk is highest just before or during the first fever, through sexual contact, kissing, or sleeping in the same room.
In 2018-2019, an outbreak in Epuyén, Argentina, produced 34 infections and 11 deaths through person-to-person contact. Sexual partners of infected people had a 17.6% secondary attack rate, compared to 1.2% for other household contacts. A 2021 review called the overall evidence for person-to-person spread “weak” and “limited to some parts of Argentina and Chile.” No other hantavirus strain has been shown to pass between people.
The virus makes blood vessels leak, and the immune system makes it worse.
Hantavirus attacks the lining of small blood vessels, making them leak. In the lung form, fluid seeps into the air spaces in the lungs. In the kidney form, the kidneys are damaged and can stop working. The body’s own immune response adds to the damage. Patients often develop low platelet counts, which means their blood doesn’t clot well.
HPS (the lung form)
HPS progresses through stages:
First stage (2-7 days): Fever, muscle aches, headache, chills, stomach pain, nausea. It looks like the flu. This is when misdiagnosis is most likely and most dangerous.
Second stage: A sudden shift to coughing, trouble breathing, fast heartbeat, and falling blood pressure. The lungs fill with fluid. This transition can happen within hours. Most deaths occur in the first 24 hours after hospital admission.
Recovery: For survivors, recovery takes weeks to months. Some patients have lingering fatigue and reduced exercise tolerance.
HFRS (the kidney form)
HFRS passes through five phases: fever, low blood pressure, decreased urine output, increased urine output, and recovery. Symptoms include high fever, headache, back and stomach pain, and bleeding (such as nosebleeds). Some patients need dialysis to clean their blood when the kidneys fail.
890 cases in 30 years, almost all west of the Mississippi.
Since 1993, the United States has recorded 890 confirmed cases of hantavirus pulmonary syndrome. About 30 per year. 96% occurred west of the Mississippi. New Mexico and Colorado have the highest counts.
70% to 80% of patients are men. The average age is 34.
Occupations with higher risk:
Forestry workers face the highest occupational risk, 2.9 times the odds of infection compared to the general population.
Farmers are at 1.9 times the risk.
Construction workers, especially those demolishing old buildings.
Military personnel training outdoors.
Anyone cleaning enclosed spaces — cabins, sheds, barns, basements — that have been closed up and occupied by rodents.
About 40% of U.S. patients reported direct rodent contact or cleaning a rodent-affected area before getting sick.
Other risk factors:
Living in rural areas, which increases both exposure and the time it takes to reach a hospital.
Living in dry areas, especially in the western U.S.
Smoking has been linked to one type of hantavirus in Europe.
Certain genes that affect the immune response may increase severity.
One pattern scientists have noticed: in places where many people have been exposed to hantavirus over time, like Paraguay and Panama, where seroprevalence runs 17% to 40%, people tend to get milder disease. In places where fewer people have been exposed, like the U.S., Chile, and Argentina, where seroprevalence is under 3%, disease tends to be more severe.
The most important diagnostic question: have you been around mice or rats?
Diagnosing hantavirus early is difficult. The first few days look like the flu, COVID, or many other infections. The critical clue is a history of rodent exposure combined with rapid respiratory decline and a low platelet count.
Doctors use blood tests to look for antibodies against the virus or for the virus itself. They also look for a rising hematocrit (red blood cell concentration) and unusual white blood cells. If initial tests come back negative, repeat testing 72 hours after symptom onset is recommended.
Asking the patient about recent contact with rodents or rodent-affected spaces is one of the most important steps in making the diagnosis.
There is no cure. Survival depends on ICU support and timing.
There is no cure for hantavirus. Treatment is supportive, meaning doctors manage symptoms and keep the body functioning while the immune system clears the virus.
Standard care includes:
IV fluids, with careful monitoring of electrolytes
Medicines to support blood pressure
Supplemental oxygen
Mechanical ventilation (a breathing machine) for severe cases
Dialysis if the kidneys fail
For the most severe cases: Extracorporeal membrane oxygenation (ECMO) can take over for the heart and lungs. When started early, before full cardiovascular collapse, survival rates with ECMO are around 80%. ECMO requires a specialized team and equipment found at major medical centers.
Experimental treatments under investigation:
Convalescent plasma, blood products from people who have recovered, showed lower death rates in an open study in Chile for Andes virus infections.
Monoclonal antibodies are being tested.
Favipiravir, an antiviral drug, showed promise in animal studies when given before the virus spread widely in the body.
Treatments that did not work: Ribavirin showed no benefit for the lung form. Methylprednisolone, a steroid, also failed to improve outcomes.
Rodent-proofing is cheap, proven, and more reliable than protective gear.
Prevention comes down to two things: keeping rodents out of buildings, and cleaning safely when rodent contamination is present.
Keeping rodents out
Seal any opening larger than a quarter inch with steel wool, metal mesh, or caulk.
Store all food, including pet food, in thick, sealed containers.
Remove woodpiles, brush, and clutter from around the outside of buildings.
Use snap traps for ongoing rodent control.
Rodent-proofing works. In studies, sealed buildings had significantly fewer rodent infestations. A program in a Native American community in New Mexico dramatically reduced rodent activity. After the 2012 Yosemite outbreak — 10 visitors infected, 3 dead from staying in cabins with mouse-infested insulation — the park sealed structures and reduced the deer mouse population over the next six years.
Cleaning rodent-contaminated areas
Open windows and doors for at least 30 minutes before entering.
Never sweep or vacuum dry rodent droppings. This is the most common way the virus gets into the air.
Spray surfaces with a 10% bleach solution and let it sit for at least 10 minutes.
Wipe up with a wet mop or sponge.
Wear rubber gloves and a properly fitted N95 mask.
Double-bag dead rodents and contaminated waste.
For workers in high-risk jobs
Training on hantavirus risk and recognition.
Proper protective equipment.
Written cleaning procedures for rodent-contaminated areas.
Knowledge of early warning signs.
Studies show that even trained workers don’t always follow safe cleaning practices, particularly when they encounter rodents unexpectedly. This is why keeping rodents out of buildings in the first place matters more than relying on protective gear alone.
Each outbreak revealed something new about how the virus spreads.
Four Corners, 1993: The outbreak that put hantavirus on the map in the Americas. A cluster of deaths in the Southwest led to the discovery of Sin Nombre virus in deer mice. Scientists later linked the outbreak to an El Niño cycle that had boosted vegetation, thereby increasing the mouse population and human exposure.
Yosemite, 2012: Ten visitors contracted Sin Nombre virus; three died. Nine of the ten had stayed in tent cabins with foam insulation that attracted nesting deer mice. 14% of trapped mice in the cabin area carried the virus. All 91 tent cabins were dismantled.
Epuyén, Argentina, 2018-2019: The largest documented person-to-person hantavirus outbreak. Thirty-four infections, 11 deaths. Researchers identified super-spreaders and confirmed transmission through close contact, particularly among sexual partners.
Gene Hackman household, 2025: Betsy Arakawa, wife of actor Gene Hackman, died of hantavirus in their home, where investigators found rodent infestation. Despite prolonged close-quarters exposure, Hackman did not contract the virus, a reminder that even sustained household contact does not guarantee transmission with non-Andes strains.
Animal-waste diseases cause 450,000 infections in the U.S. each year.
Hantavirus is one of many illnesses people catch from animal urine, droppings, and saliva. In total, animal-contact illnesses cause roughly 450,000 infections, 5,000 hospitalizations, and 76 deaths in the United States each year.
Salmonella from backyard chickens is now the leading source of animal-contact salmonella in the U.S. Between 2009 and 2021, nearly 9,000 outbreak-linked illnesses, close to 1,800 hospitalizations, and 15 deaths were reported across all 50 states.
Leptospirosis is a bacterial infection spread through rodent and dog urine. Over 1,000 U.S. cases were reported between 2014 and 2020. The fatality rate is 10%. Cases are rising, particularly in New York City’s Bronx borough and in Hawaii, Puerto Rico, and the Southeast after flooding events.
Histoplasmosis is caused by fungal spores in soil enriched by bat and bird droppings. In the Ohio and Mississippi River valleys, 60% to 90% of residents have been exposed. Most cases are mild or asymptomatic, but it can be fatal for immunocompromised people.
Tularemia from rabbits and rodents rose 56% during the 2010s. About 100 to 250 cases per year, concentrated in Arkansas, Missouri, Kansas, and Oklahoma.
Plague still occurs in the rural Southwest — a few cases per year from flea bites on infected rodents.
Cryptosporidium and E. coli from cattle are common at petting zoos and farms.
Toxoplasmosis from cat feces poses particular risks for pregnant women.
The pattern across these diseases is similar. The mechanisms are understood. The prevention is largely structural: housing quality, pest control, sanitation, and occupational safety. The populations most at risk tend to have the least access to those protections.
The agency responsible for tracking these diseases lost a third of its staff.
The CDC is the primary federal agency responsible for tracking and investigating these diseases.
As part of a broader HHS restructuring, the CDC’s workforce was cut by about 2,400 employees. Former officials have said the agency lost about 3,000 people overall through layoffs, buyouts, and resignations. The Epidemic Intelligence Service, the CDC’s outbreak investigators, was initially threatened with cuts but ultimately spared, and a new class was exempted from the hiring freeze. In October 2025, about 1,000 CDC employees received reduction-in-force notices. Roughly 600 remained terminated after hundreds of notices were reversed.
The CDC's Vessel Sanitation Program, which handles cruise ship health inspections, lost all of its full-time civilian employees before being reinstated when the National Center for Environmental Health was restored. The HHS Office of Infectious Disease and HIV/AIDS Policy, which oversaw the Ending the HIV Epidemic initiative and childhood vaccination efforts, was eliminated. Three of 20 port health stations now have no staff.
In January 2026, the United States completed its withdrawal from the World Health Organization, a process the White House initiated a year earlier. HHS and the State Department also rejected the amended International Health Regulations, the framework countries use to share information about cross-border outbreaks. The administration is now proposing to spend $2 billion a year to rebuild the global disease surveillance and outbreak response functions the U.S. previously accessed through WHO at a fraction of that cost.
These changes affect the country’s capacity to detect, investigate, and respond to outbreaks of hantavirus and the broader category of animal-waste diseases described above.
The bottom line on hantavirus risk and prevention.
Hantavirus is rare in the United States, about 30 cases per year, but it is one of the deadliest viral infections a person can contract, with a fatality rate of 36% to 38% for the lung form.
There is no vaccine and no antiviral treatment. Survival in the worst cases depends on reaching an ICU with ECMO capability quickly.
The best prevention is keeping rodents out of buildings and never sweeping or vacuuming dry rodent waste. These measures are proven and low-cost.
Hantavirus is part of a broader group of diseases spread through animal waste. Taken together, these diseases cause roughly 450,000 illnesses in the U.S. each year. The prevention for most of them is structural — housing quality, pest control, sanitation, and occupational safety.
The public health infrastructure responsible for tracking and investigating these diseases has been significantly reduced over the past year.