A New Tylenol Study Doesn’t Show What the Headlines May Claim
A study of 2 million births finds small associations that disappear when siblings are compared — the same pattern seen in earlier research.
Is Tylenol linked to autism?
A new analysis in JAMA Pediatrics, based on more than 2 million births in Taiwan, is the latest to revisit the question.
If you only read the headlines, you might think the science has suddenly changed.
It hasn’t.
Like a massive Swedish study published in JAMA in 2024, the new paper finds small associations that disappear once researchers account for family factors.
Which is another way of saying: the data still don’t show that acetaminophen causes autism or ADHD.
What the Taiwan study brings to the table
Three things stand out.
First, the scale. Researchers analyzed 2,092,926 births in Taiwan between 2004 and 2015. That’s a lot of babies.
Second, the familiar pattern. When researchers compared unrelated children, they saw a small statistical association between acetaminophen use during pregnancy and ADHD or autism. But when they compared siblings born to the same mother, that association disappeared.
Third, a new puzzle. When the researchers dug deeper into the sibling analysis, the results flipped depending on which sibling was exposed. That kind of reversal usually signals bias in the data, not a drug effect.
The small signal that keeps showing up
In the Taiwan study, children whose mothers were prescribed acetaminophen during pregnancy had slightly higher rates of:
ADHD (about a 12% relative increase)
Autism (about a 6% relative increase)
Those numbers may sound alarming.
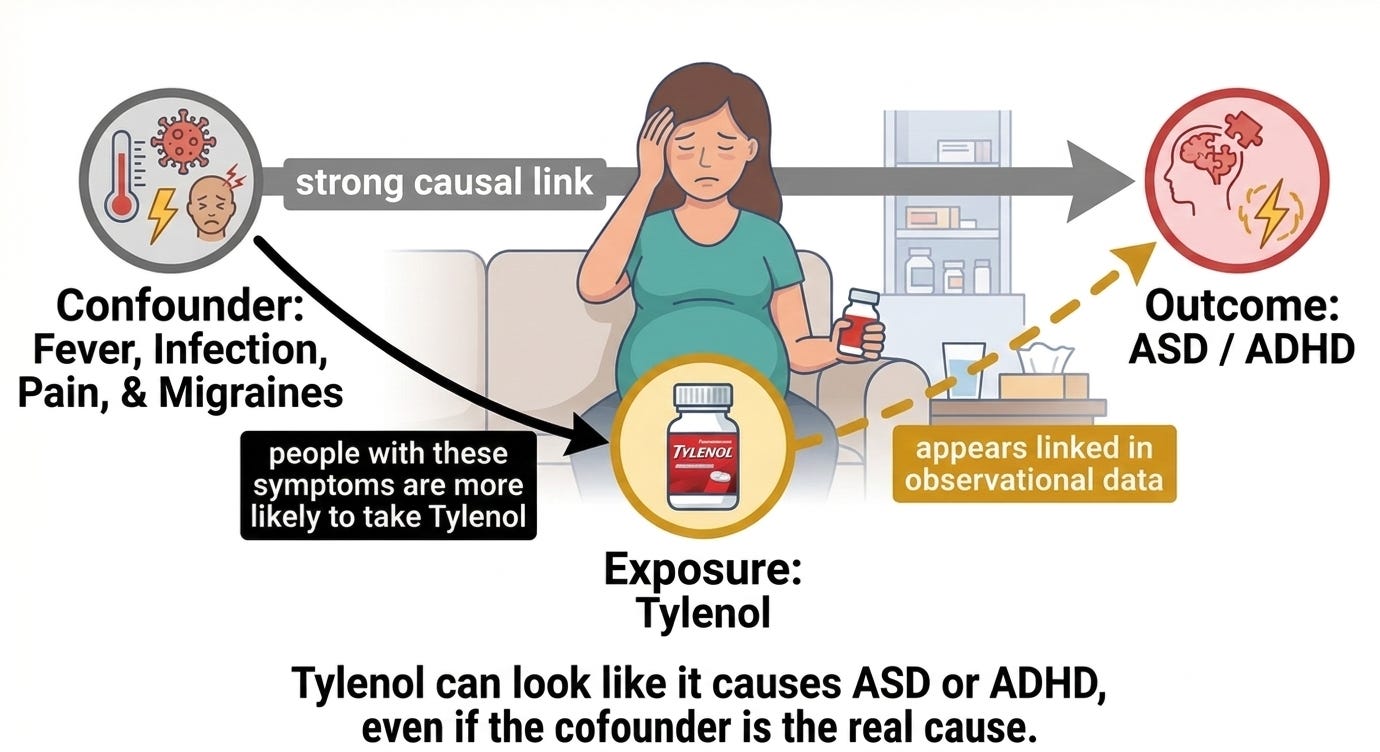
But in epidemiology, small associations like this often turn out to be confounding. In other words, something else explains the relationship. And in this case, there’s an obvious candidate.
People don’t usually take acetaminophen during pregnancy for fun. They take it because they have:
fever
infection
migraines
pain
Some of those conditions may themselves affect fetal development.
This is called confounding by indication, one of the oldest headaches in drug safety research.
Trying to separate family factors from drug effects
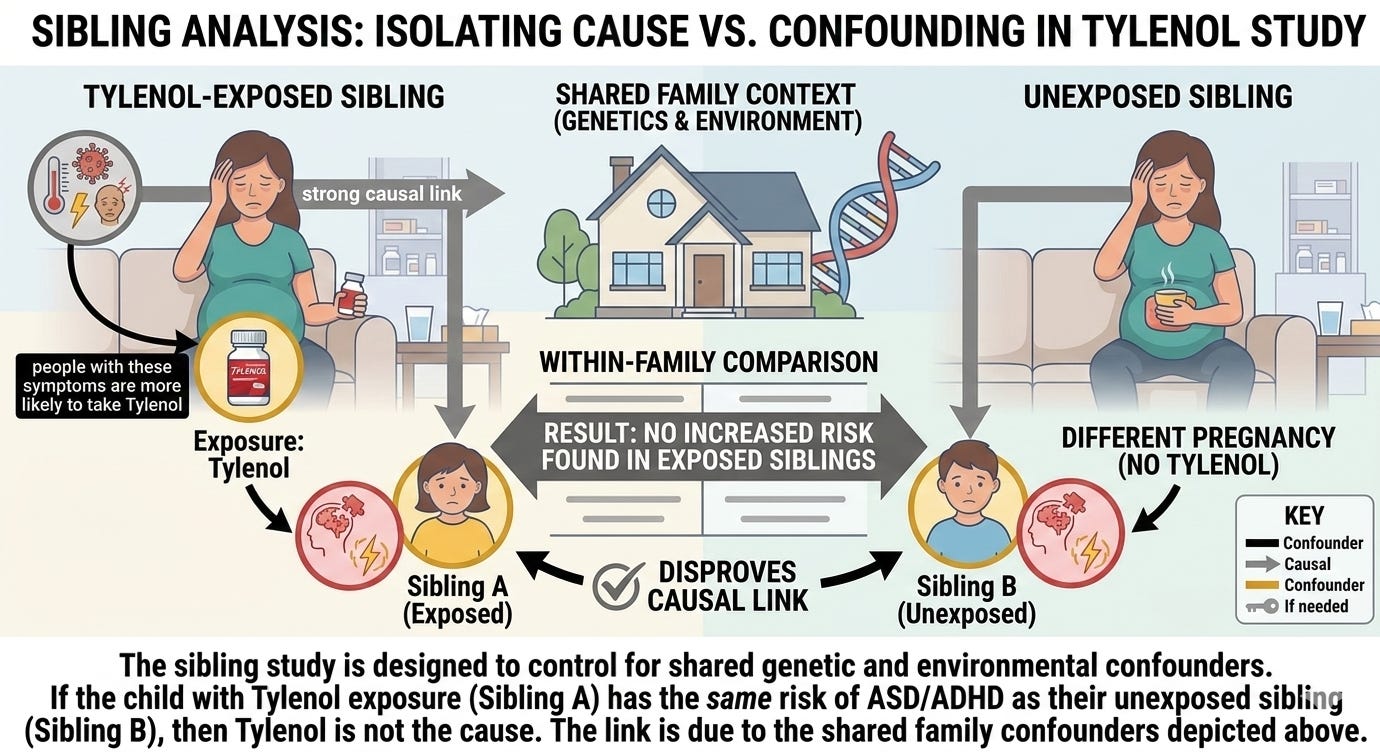
To try to untangle that problem, researchers sometimes compare siblings born to the same mother.
The idea is simple. Siblings share a lot:
genetics
home environment
parental traits
socioeconomic background
So if one sibling was exposed to a medication during pregnancy and the other wasn’t, that comparison can help remove some sources of bias.
This approach has become central to the Tylenol debate.
What the Swedish study already showed
In 2024, researchers in Sweden published one of the largest sibling studies ever done on this question. They followed 2.48 million children.
At first glance, the results looked familiar. In standard population analyses, acetaminophen use during pregnancy appeared linked to slightly higher risks of autism, ADHD, and intellectual disability.
But when researchers compared siblings, the associations essentially vanished. The hazard ratios hovered around 1.0. In plain English: no meaningful difference.
The Swedish researchers concluded that the earlier signals likely reflected family-related factors rather than the medication itself.
The Taiwan study finds the same pattern
The new Taiwan study reaches almost the same conclusion.
When researchers compared unrelated children, they saw small associations.
When they compared siblings, those associations disappeared.
But the Taiwan researchers went a step further. And that’s where things got interesting.
When the data stop making biological sense
The researchers separated families into two groups: families where only the older sibling was exposed to acetaminophen, and families where only the younger sibling was exposed.
If the drug truly increased risk, the direction of the association should stay the same. But it didn’t. When the older sibling was exposed, the association looked positive. When the younger sibling was exposed, the association flipped negative. That’s not how biology usually behaves. But it’s exactly what you might expect if bias is still lurking in the data.
Possible explanations include:
changes in autism and ADHD diagnosis over time
differences in follow-up between siblings
birth-order effects
pregnancy-specific health differences
The authors themselves concluded that the contradictory results likely reflect unaddressed sources of bias.
In other words: the data are messy, which is pretty normal for large observational studies.
The sibling-study debate
Sibling studies are often seen as one of the stronger tools we have in observational research. But they’re not perfect. NIH Director Dr. Jay Bhattacharya has pointed out several limitations.
First, sibling analyses include only families in which exposure differs between pregnancies — so-called discordant siblings. Those families may not represent the broader population.
Second, restricting the sample this way shrinks the dataset, which can reduce statistical power.
Third, sibling designs control for family-level factors but not pregnancy-specific ones, like infections or fever — the very reasons someone might take acetaminophen.
And finally, acetaminophen is widely taken over the counter, which means medical records may miss some exposures.
These are reasonable concerns. But they apply to many observational studies, not just sibling designs. And when multiple large studies from different countries show the same overall pattern, that matters.
The Texas lawsuit over Tylenol
While scientists debate how to interpret these findings, the issue has also moved into the courts.
Earlier this year, Texas Attorney General Ken Paxton sued Johnson & Johnson and Kenvue, the company that now sells Tylenol.
The lawsuit claims the companies misled consumers by failing to warn that taking acetaminophen during pregnancy could increase the risk of autism or ADHD.
A Texas judge recently rejected Kenvue’s motion to dismiss the case, allowing the lawsuit to move forward.
But the legal question is different from the scientific one. Courts focus on whether companies disclosed potential risks. Scientists focus on whether a causal relationship has actually been proven.
Most major medical groups — including the American College of Obstetricians and Gynecologists (ACOG) — say the current evidence does not establish that acetaminophen causes autism or ADHD. ACOG reaffirmed in 2025 that acetaminophen remains one of the safest options available to treat pain or fever during pregnancy.
Still, lawsuits can shape public perception. For many families, seeing a lawsuit filed can sound like proof that the science is settled. In reality, it isn’t.
What pregnant patients should know
Acetaminophen remains one of the most widely used and best-studied medications during pregnancy. It’s often taken to treat fever or severe pain — conditions that can themselves pose risks to the baby if left untreated.
The new study does not show that acetaminophen causes autism or ADHD.
Instead, it highlights something less dramatic but more important: when scientists study very small risks in very large datasets, the results can be messy. That’s the nature of observational research.
Progress tends to come slowly, across many studies, rather than from a single headline-grabbing paper. Which may not be exciting. But it’s how science works.