The Market for Reassurance in Cancer Screening
A major trial failed to show fewer late-stage cancers. So why are we so eager to buy tests that reassure us?
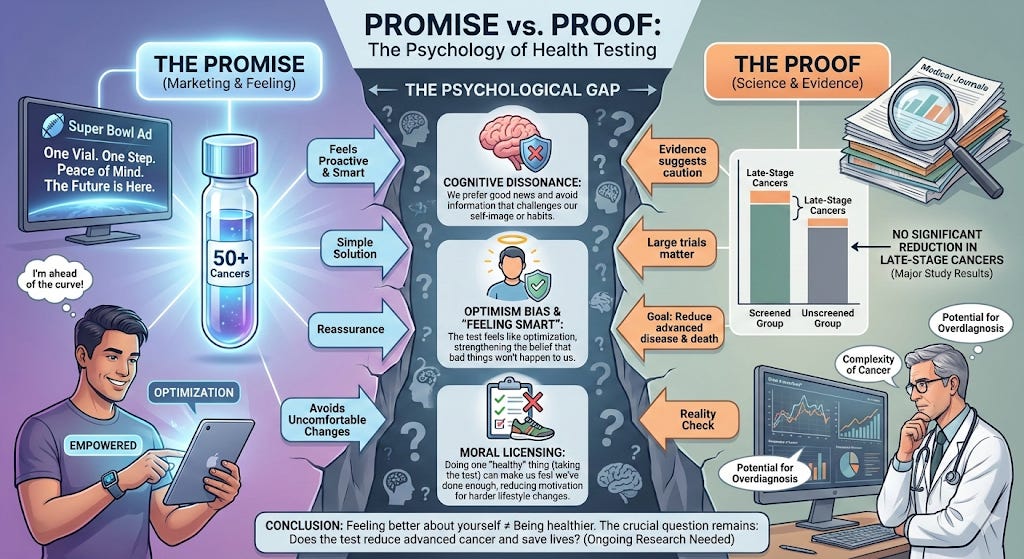
Promise vs Proof
During the Super Bowl, a sleek ad made a powerful promise. Wealthy people live longer because they invest in their health. A simple blood test could look for more than 50 cancers at once. Just one vial. Just one step. Peace of mind.
It sounded like the future.
A couple of weeks later, the science told a more complicated story.
In a major study of 142,000 people in England, the Galleri blood test did not significantly reduce the number of late-stage cancers, which was the main goal of the trial. The idea behind the test is simple: find cancer early, before it spreads. But in this large, carefully designed study, the test did not clearly lower the number of advanced cancers compared with people who did not get the test.
And yet, the test has already been sold to hundreds of thousands of Americans for about $1,000 each.
The gap between the excitement and the evidence raises a bigger question: why are we so eager to buy health tests that make us feel better about ourselves, even when we do not yet know if they make us healthier?
What cancer screening is supposed to do
Cancer screening isn’t just about finding cancer. It’s about saving lives.
For a screening test to truly help, it needs to actually reduce the risk of advanced cancer disease or death. Finding more cancers isn’t enough. Some cancers grow slowly and may never cause harm (i.e. you die with the cancer, not from the cancer). Others are aggressive and may spread before any test can catch them.
That is why large trials matter. They tell us whether a test changes what counts.
In this case, the early results suggest caution.
Why reassuring tests are so appealing
Psychology helps explain why a test like this can be so attractive.
For decades, researchers have shown that people prefer information that makes them feel good about themselves. When we hear something that suggests we may be unhealthy or making bad choices, we don’t like it. Psychologists call this “cognitive dissonance.” We often respond not by changing our behavior, but by avoiding or questioning the threatening information.
Studies show that people are more likely to accept medical test results that reassure them and more likely to doubt results that suggest a problem. Other research shows that people sometimes avoid medical information altogether if they fear it will be upsetting.
In simple terms: we like good news. We resist bad news.
A test that says, “You’re proactive. You’re ahead of the curve. You’re taking control,” fits neatly into that preference. We want to feel good about what we’re already doing. We may not want to hear that we should do something else.
Feeling smart feels safe
There is another layer.
Research shows that people often use their feelings as shortcuts. If something feels empowering, modern, and responsible, we are more likely to believe it is valuable.
A sleek blood test marketed during the Super Bowl does not feel like an illness. It feels like optimization. It feels like something smart people do.
There is also something called optimism bias. Most of us believe bad things are more likely to happen to other people than to ourselves. A broad cancer test does not challenge that belief. Instead, it strengthens it. It says: you’re staying ahead.
And once we take a step that feels healthy, we may feel less pressure to make harder changes, like exercising more, drinking less alcohol, or losing weight. Psychologists call this “moral licensing.” Doing one good thing can make us feel we have done enough.
The market for reassurance
Modern healthcare isn’t just about medicine. It’s also about identity.
Some tests demand action. A high blood pressure reading, for example, may mean lifestyle changes or medication. These actions can be uncomfortable, inconvenient, and disruptive.
Other tests offer reassurance. They tell you that you are responsible and forward-thinking. They do not immediately require change.
The market often rewards the second kind.
That does not mean the technology is useless. It means the psychology is powerful.
Multi-cancer blood tests may eventually prove helpful. Ongoing research may show clearer benefits over time.
But the central question remains simple: Does the test reduce advanced cancer and save lives?
That question matters more than how modern, empowering, or impressive the test feels.
In healthcare, feeling better about yourself and being healthier aren’t always the same thing.